Hysteroscopy Surgery
- Home
- Hysteroscopy Surgery
Hysteroscopic surgery is an incisionless, minimally invasive gynecologic procedure that allows surgeons to visualize the uterus. It is performed using a thin, lighted, camera-equipped tube called a hysteroscope. The hysteroscope allows surgeons to clearly visualize and examine the cervix and inside of the uterus.
Hysteroscopy is primarily used to diagnose and treat the causes of abnormal uterine bleeding. Although it is generally considered an outpatient procedure, it can also be performed in the office setting for simple cases.
Overall, hysteroscopic surgery represents a modern and safe approach for diagnosing and treating intrauterine conditions without external incisions or visible scarring.
What Is Hysteroscopic Surgery?
Hysteroscopic surgery is a minimally invasive, incisionless procedure performed to diagnose and treat conditions affecting the uterus.
Unlike traditional gynecological surgeries, it does not require abdominal incisions. The procedure uses a thin, lighted, flexible tube called a hysteroscope, which is equipped with a high-resolution camera.
The hysteroscope is gently inserted through the vagina and cervix, allowing surgeons to directly visualize the uterine cavity on a monitor in real time.
Hysteroscopic surgery can be performed under different types of anesthesia, depending on the complexity of the procedure.
When Is Hysteroscopic Surgery Recommended?
Hysteroscopic surgery is recommended in these conditions:
| case | details |
|---|---|
| Endometrial polyps | Small, non-cancerous growths in the lining of the uterus |
| Abnormal uterine bleeding | Heavy, irregular, or prolonged menstrual periods |
| Postmenopausal bleeding | Vaginal bleeding occurring after the last menstrual period |
| Retained pregnancy tissue | Fetal or placental tissue that remains in the uterus after miscarriage, or childbirth |
| Uterine septum | A small band of the tissue dividing the uterus, which can affect fertility or pregnancy |
| Submucosal fibroids | Fibroids in the inside cavity of the uterus |
| Asherman’s syndrome | Intrauterine adhesions |
| Uterine synechiae | Scar tissue inside the uterine cavity |
Types of Hysteroscopic Surgery
Hysteroscopy can be part of both the diagnostic process and the treatment process. There are two main types of hysteroscopic surgery:
1. Diagnostic Hysteroscopy
What is Diagnostic Hysteroscopy?
Diagnostic hysteroscopy is a commonly performed gynecologic procedure used to evaluate the endometrial cavity. It helps identify structural abnormalities in the uterus that may be responsible for abnormal uterine bleeding or other gynecologic symptoms.
Indications for Diagnostic Hysteroscopy
Diagnostic hysteroscopy is used to examine and directly visualize the uterine cavity, including:
- The endocervical canal.
- The endometrial cavity.
- The tubal ostia (opening of the fallopian tubes).
- Suspected blockage of the fallopian tubes.
- Detection of isthmocele (cesarean scar defect)
- Suspicion of endometrial malignancy.
Diagnostic hysteroscopy may also help confirm the findings of other imaging studies, such as ultrasound or hysterosalpingography.
Key features of Diagnostic Hysteroscopy
Diagnostic hysteroscopy is a minimally invasive procedure with the following advantages:
- Low-risk procedure.
- Incisionless technique.
- Can be performed in an office or outpatient setting.
- Quick recovery.
- Short procedure time.
2. Operative Hysteroscopy
What is Operative Hysteroscopy?
Operative hysteroscopy is a therapeutic procedure used to treat abnormalities detected during diagnostic evaluation. In many cases, diagnostic and operative hysteroscopy can be performed during the same session, allowing both identification and treatment of the condition.
Indications of operative hysteroscopy
Operative hysteroscopy can be performed in a wide range of uterus conditions, including:
- Removal of endometrial polyps.
- Removal of submucosal fibroids.
- Removal of retained pregnancy tissue.
- Removal of intrauterine foreign bodies.
- Treatment of isthmocele.
- Treatment of intrauterine adhesions (Asherman's syndrome)
- Correction of congenital uterine anomalies.
- Resection of a septate uterus.
Diagnostic vs Operative Hysteroscopy
There are two main types of hysteroscopy, and they may be performed during the same surgical session if needed. The basic differences between diagnostic and operative hysteroscopy include the following:
| Comparison | Diagnostic Hysteroscopy | Operative Hysteroscopy |
|---|---|---|
| Procedure Duration | 5 – 15 minutes | 30 -60 minutes |
| Purpose | Observation or detection of uterine abnormalities | Removing or treating uterine abnormalities |
| Equipment | Hysteroscope only | Hysteroscope with additional surgical instruments |
| Anesthesia | Mild sedation or local anesthesia | Deeper sedation or general anesthesia |
| Risk level | Very low complication rate | Very low complication rate, slightly higher than diagnostic hysteroscopy |
| Setting | May be performed in an examination room or outpatient clinic | Usually performed in an outpatient center and may require an operating room |
Diagnostic and operative hysteroscopy can be performed during the same procedure, which may make the total surgical time longer compared to performing each procedure separately.
Both types involve the insertion of a camera-equipped hysteroscope through the cervix to visualize the uterine cavity.
How to Prepare for a Hysteroscopic Surgery?
Before Procedure
Dr. Talal Al-Nukari’s recommendations for patients before undergoing hysteroscopic surgery include the following:
- Do not eat or drink anything after midnight the night before, unless instructed otherwise.
- Inform Dr. Talal of all medications you are currently taking, especially blood thinners or hormonal treatments.
- A preoperative evaluation and any necessary investigations will be arranged according to the patient's individual needs.
- Hysteroscopy may be performed at any time in postmenopausal women. However, in premenopausal women, it is preferably performed outside the secretory phase of the menstrual cycle, as this phase may increase the possibility of overdiagnosing endometrial polyps.
- A preoperative pregnancy test should be performed on all premenopausal women prior to hysteroscopy.
- Wear loose, comfortable clothing on the day of the procedure and avoid wearing jewelry.
- Arrange for someone to drive you home after the procedure due to anesthesia.
Following these instructions helps ensure a safe procedure, faster recovery, and better outcomes.
After procedure
- If your hysteroscopic surgery is performed under anesthesia, you may be medically observed in the recovery room for several hours.
- Some cramping or light vaginal bleeding for a few days is normal.
- Hysteroscopy is a minor procedure and usually does not require an overnight hospital stay. Most patients can return home a few hours after surgery.
- Most patients can resume normal activities at work or home the next day of the procedure.
- It is recommended to rest well for at least 24 hours after surgery.
- Use pads for light bleeding and avoid using tampons.
- Take a pain reliever for soreness as advised.
How Long Does Hysteroscopic Surgery Takes?
The duration of a hysteroscopic procedure depends on its type and complexity.
- Diagnostic hysteroscopy is usually quick, typically takes 5 -20 minutes.
- Operative hysteroscopy may take longer, usually around 30 – 60 minutes.
- When both diagnostic and operative hysteroscopy procedures are performed simultaneously, the total time usually about 1–2 hours.
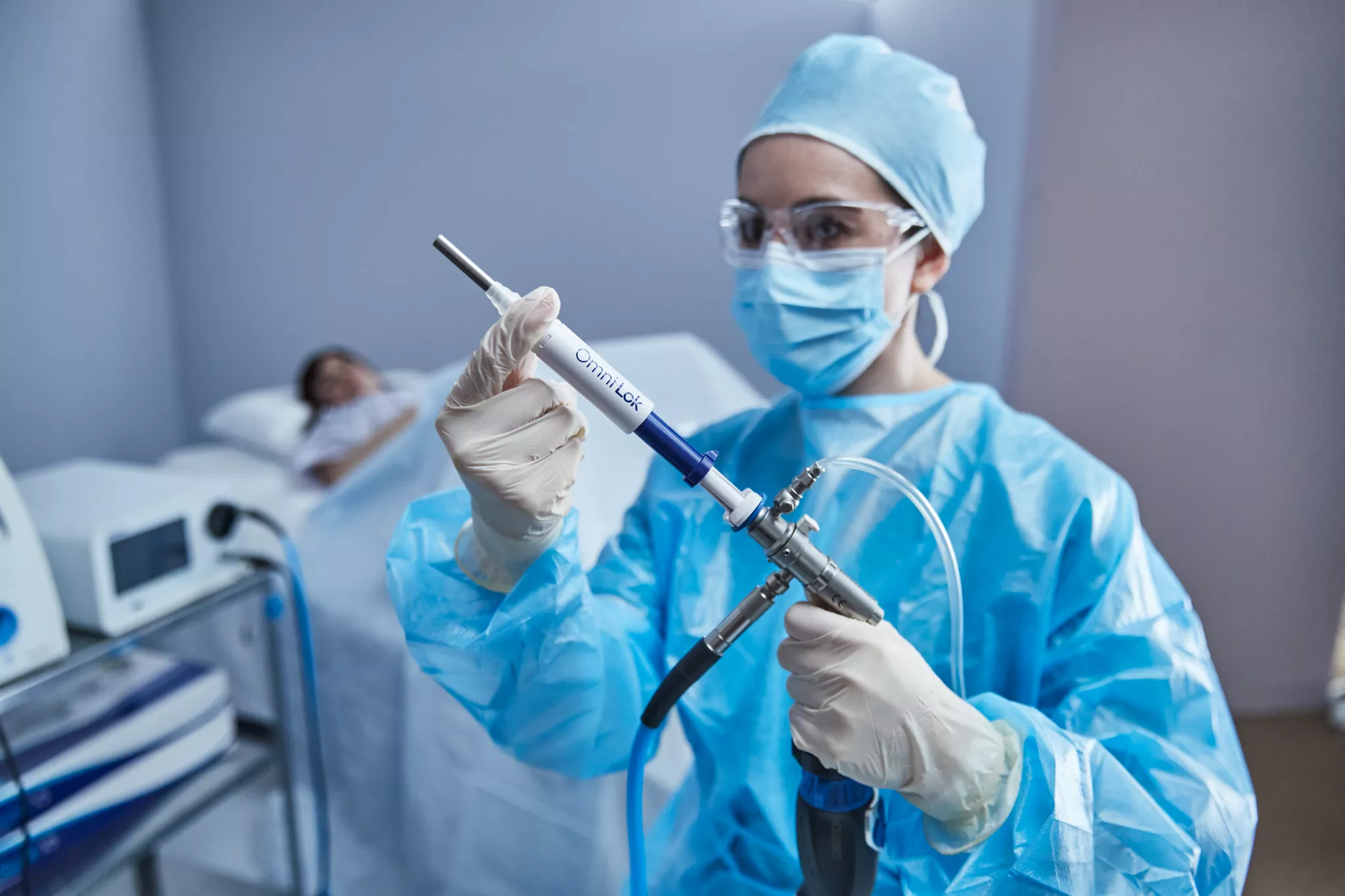
How Is Hysteroscopic Surgery Performed?
The procedure is typically performed through the following steps:
- A speculum – an instrument used to gently hold open the walls of the vagina – is inserted into the vagina.
- The cervix may be gently dilated to allow the safe insertion of the hysteroscope.
- The camera-equipped hysteroscope is carefully inserted through the cervix into the uterine cavity.
- The surgeon directly visualizes the inside of the uterus on a monitor in real time.
- Carbon dioxide gas or a sterile fluid, such as saline solution, is introduced through the hysteroscope to expand the uterine cavity and provide a clearer view.
- The expansion allows the surgeon to clearly examine the uterine lining and the openings of the fallopian tubes (tubal ostia).
- After a thorough examination, diagnostic findings are recorded, or therapeutic treatment is performed if indicated.
- Once the procedure is completed, the hysteroscope and any additional surgical instruments are carefully removed.
- The patient is then monitored for a short period before being discharged.
Is Hysteroscopic Surgery Safe?
Hysteroscopic surgery is generally considered a safe, low-risk procedure with a quick recovery. As with any surgery, complications can occur. Less than 1% of hysteroscopic surgeries can have complications; therefore it is considered a safe and well-tolerated procedure.
Hysteroscopic surgery is an incisionless, minimally invasive technique, which significantly reduces the risks compared to traditional open surgery.
Risks of Hysteroscopic Surgery
Although hysteroscopic surgery is regarded as a safe, minimally invasive procedure, complications can occur in less than 1% of cases. Potential risks include:
- Uterine perforation: The most common procedural complication, which involves a small tear in the uterine wall.
- Infection: Such as endometritis or urinary tract infections.
- Fluid overload: Excessive absorption of the distending fluid used during the procedure.
- Air and gas embolism: A rare complication that may result from the introduction of carbon dioxide (CO2) as a hysteroscopic distending medium.
- Vasovagal reaction: Symptoms may include nausea, vomiting, diaphoresis, pallor, or loss of consciousness.
- Excessive bleeding: More likely in operative procedures.
Overall, hysteroscopic surgery remains a safe procedure with a very low complication rate (less than 1%), no external scars, short operative time, and rapid recovery.
Advantages of Hysteroscopic Surgery
Hysteroscopic surgery is a modern, minimally invasive procedure that offers several advantages compared to traditional gynecologic surgery:
- Dual benefit: hysteroscopy allows surgeons to diagnose and treat uterine conditions during the same procedure.
- Minimally invasive technique it enables precise identification and removal of abnormalities without damaging the surrounding tissues.
- Incisionless procedure: The hysteroscope is inserted through the vagina without the need for abdominal incisions.
- Fast recovery: Most patients return home a few hours after surgery and resume their daily activities the following day.
- Accuracy and precision: Hysteroscopy uses a high-resolution camera installed at the top of the hysteroscope, allowing accurate and targeted treatment
- Less postoperative pain: Patients usually experience mild to moderate discomfort on the day of surgery. Compared to traditional open surgery, hysteroscopy is associated with significantly less pain.
- Low-risk: hysteroscopy is considered a safe procedure, with a very low rate of complications less than 1%.
Recovery After Hysteroscopic Surgery
The recovery process after hysteroscopic surgery is usually short and simple, and it typically goes through the following phases:
| Time Slot | Patient Condition |
|---|---|
| First 2 – 4 hours | The patient remains under medical supervision until the effects of anesthesia wear off and her condition is stable |
| First 24 hours | Mild cramping, discomfort, and light vaginal bleeding may occur |
| Next few days | Mild discomfort or light vaginal discharge may be experienced |
| After 1 week | Most patients experience complete recovery, especially after diagnostic hysteroscopy |
Hysteroscopic Surgery costs at Dr. Talal Al-Nukari's Clinic
At Dr. Talal Al-Nukari’s Clinic, the cost of hysteroscopic surgery varies depending on several factors. The total cost is determined by:
- Type of procedure: Diagnostic hysteroscopy generally costs less than operative hysteroscopy.
- Complexity of the case: operative hysteroscopy may vary depending on the patient's condition.
- Anesthesia type: Local anesthesia, sedation, or general anesthesia can affect the overall cost.
- Insurance coverage: Many insurance plans may partially or fully cover hysteroscopic procedures.
Dr. Talal’s Clinic is fully equipped with state-of-the-art facilities to provide the highest standard of care. Each case is tailored to the patient’s individual needs. For an accurate cost estimate and personalized consultation, contact Dr. Talal Al-Nukaris’s clinic to schedule a free appointment and take the first step toward regaining control of your health.
When should you contact Dr. Talal After hysteroscopic Surgery?
Contact Dr. Talal immediately after hysteroscopic surgery if you experience any of the following symptoms:
- Heavy bleeding.
- Severe pain.
- High fever.
- Nausea.
- Vomiting.
Conclusion
Hysteroscopic surgery is a safe, modern, and minimally invasive procedure, especially when performed by a highly qualified and experienced surgeon. At Dr. Talal Al-Nukari’s Clinic, you can rest assured that you will receive comprehensive, patient-centered care in a professional and supportive environment.
With Dr. Talal’s extensive experience in minimally invasive gynecological techniques, patients can regain comfort, confidence, and control over their health.
For a safe and effective approach to your gynecologic care, contact Dr. Talal Al-Nukari’s Clinic today to schedule a consultation and take the first step toward receiving the care you deserve.
Frequently Asked Questions (FAQs)
Hysteroscopic surgery is performed to diagnose and treat various uterine conditions, including:
- Abnormal uterine bleeding.
- Endometrial polyps.
- Submucosal fibroids.
- Uterine septum.
- Retained pregnancy tissue.
- Other intrauterine abnormalities.
Most patients experience mild to moderate pain and discomfort on the day of the procedure. Compared to traditional open gynecologic surgery, hysteroscopic surgery is generally much less painful.
Common side effects of hysteroscopy include:
- Mild cramping, discomfort, or abdominal pain.
- Light vaginal bleeding for a few days.
- Temporary changes in menstrual flow.
Most patients can return home a few hours after the procedure, with rest recommendation for the first 24 hours. Light daily activities can usually be resumed within 1-2 days.
Full recovery is typically achieved within 4-6 days, especially after diagnostic hysteroscopy.
Operative hysteroscopy may require a slightly longer recovery.
No. Hysteroscopic surgery is a safe, low-risk procedure with a very low complications rate (less than 1%), it is generally regarded as a minimally invasive and well-tolerated procedure.
Doctors may recommend hysteroscopy to diagnose or treat the uterine conditions, such as submucosal fibroids, endometrial polyps, uterine synechiae, and abnormal bleeding. It may also be used to confirm findings from imaging tests like ultrasound or hysterosalpingography.
No. Hysteroscopy is generally not performed during pregnancy.
Call for a Consultation now with Dr.Talal Al Nukari

Dr. Talal Badi Al Nukari is a highly skilled and experienced Obstetrics and Gynecology Specialist with a passion for providing the best medical care to his patients.
Quick Links
Get in Touch
- +971663500168
- talal@maxhealthcare.ae
- Abu Dhabi
- Mon-Fri: 10am-06pm
Copyright 2025 © All rights Reserved.